Human Papillomavirus Infection (HPV)
Human Papillomavirus Infection (HPV): Tests and Prevention
Disclaimer: Not medical or professional advice. Always seek the advice of your physician.

Human papillomavirus (HPV) is the most common sexually transmitted infection. More than 660 million people in the world are currently infected with HPV. The virus mostly affects people under the age of 35. According to the World Health Organization, HPV-associated diseases account for more than 10% of all malignancies in the cervix, rectum, anus, larynx, pharynx, vulva, and penis.
The main route of transmission is through sexual intercourse. Correct use of condoms can significantly reduce, but not eliminate, the risk of infection. Besides, it makes no difference whether the person has visible signs of infection (condyloma) or not. Most infected people can spread the virus to others without knowing they have an infection.
HPV Types
At present, more than 200 types of HPV have been identified. They are classified into 4 groups according to the risk of cancer. Each type has a number (assigned in the order in which it was discovered).
- never cause cancer (1, 2, 3, 4, 5, 10, 28, 49)
- low-risk of cancer (6, 11, 13, 32, 40 - 44, 51, 72)
- intermediate-risk of cancer (26, 30, 35, 52, 53, 56, 58, 65)
- high-risk types that often lead to cancer (16, 18, 31, 33, 39, 45, 50, 59, 61, 62, 64, 68, 70, 73)
What Tests can Detect the Human Papillomavirus?
DNA testing by polymerase chain reaction (PCR) is a standard method for determining the presence of an HPV infection. It can be detected almost immediately after exposure. However, having an HPV-positive test does not mean that a person is sick. The virus can hide out in the body for a long time without causing disease. It can stay there in an inactive state. It is also known that not all HPV strains are dangerous. There are certain types that are referred to as oncogenic. The immune system can eliminate the infection from the body in nearly half of the cases.
HPV does not go away in all other cases. This is an important point. The longer the virus remains dormant (hidden) in the body, the higher the risk of its activation. It can consequently lead to the development of various precancerous conditions and cancer. Symptoms may or may not include growths on the skin and mucous membranes. If left untreated, the risk of cancer increases tenfold.
How to Prevent HPV-Related Cancer?
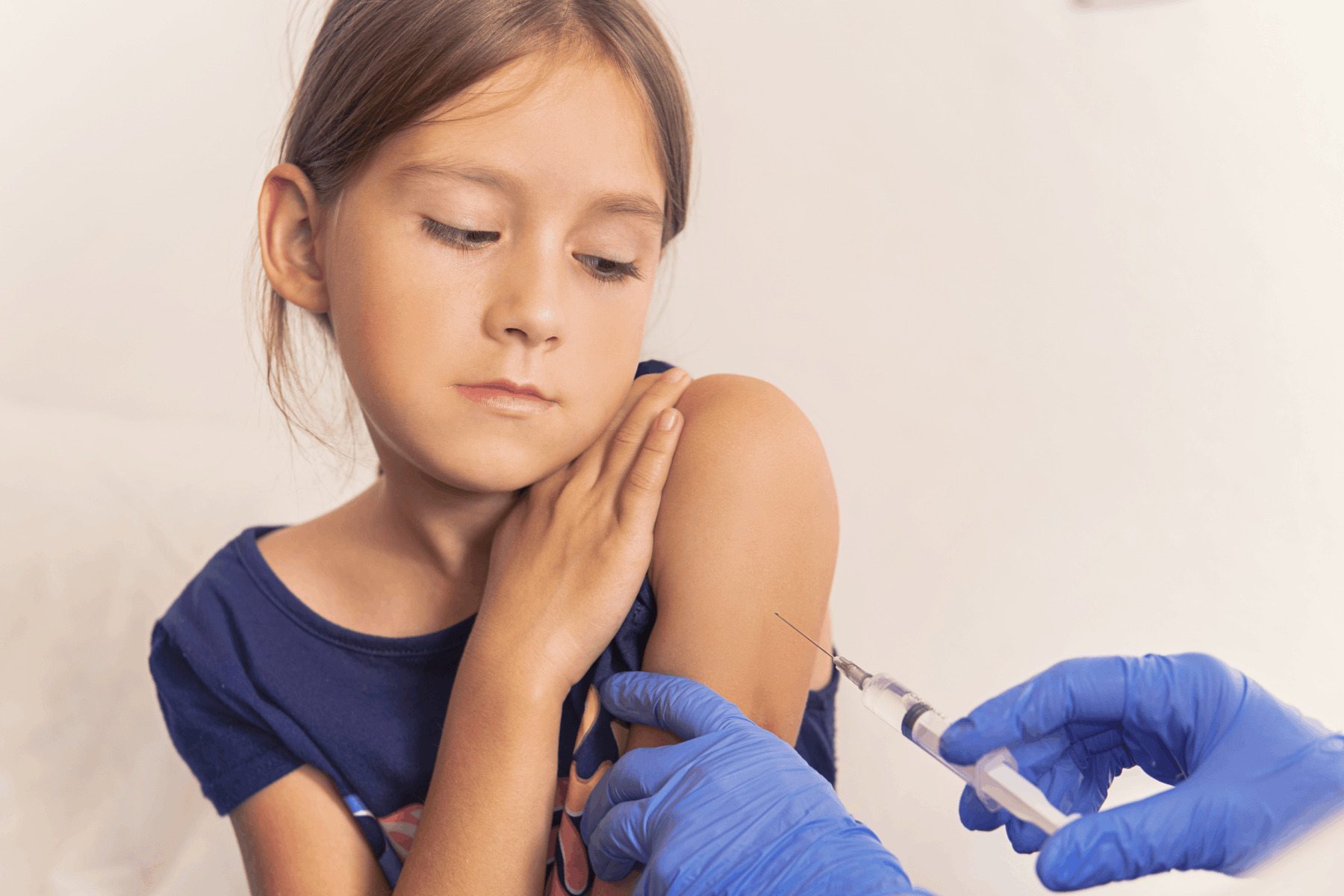
The HPV vaccine helps protect against cancer. It maintains effectiveness up to 15 years after injection. Studies show that women vaccinated 15 years ago still have enough antibodies to protect against the virus. Vaccination can be started at the age of 9.
Vaccination against papillomavirus reduces the risk of various diseases.
- Cervical cancer — The vaccine reduces the risk of the disease by approximately 70% to 90%, depending on the type of vaccine.
- Vaginal cancer — Reduces the risk by 96%.
- Rectal cancer — Reduces the risk by 77%.
- The vaccine also prevents genital and laryngeal warts that appear shortly after infection.
When Should you Get Tested for HPV?
HPV 16 and 18 are the most dangerous types of papillomavirus. They cause about 70% of HPV-related cervical cancer. Let's figure out how to prevent this from happening.
- It makes no sense to get tested for HPV if the onset of sexual activity has occurred less than 10 years. Most HPV infections clear up on their own. It is recommended to take an HPV test from the age of 25-30.
- If it has been more than 10 years since the onset of sexual activity (or you are 30), an HPV test should be taken together with a PAP test (cytological examination of a cervical smear). If HPV type 16 or 18 is detected, you should have a colposcopy.
- If HPV 16 or 18 is detected, and no changes are found in the PAP test and colposcopy, the examination must be repeated in 1 year.
- If the PAP test shows changes, you must have a biopsy. A biopsy may also be needed if there are no changes in the PAP test.
- Depending on the biopsy results, the physician will confirm a diagnosis and let you know if surgery is required.
HPV does not cause cervical inflammation/vaginal discharge/itching/burning/pain during sex. It is of no use to get an HPV test with such symptoms and manifestations. There is no cure for HPV! However, the body's immune system can get rid of the HPV infection naturally within two years (it happens in 90% of cases).
Important! Vaccination does not treat HPV. Vaccination is most reasonable before the onset of sexual activity when the infection has not yet occurred.

.png)
![Ling [Last Name]](/uploads/files/ling_(1).png)